Cancer Screening, Treatment, & 5-Year Survival - Part 2
Breast Cancer
For women, the emphasis placed on annual mammograms is significantly greater than any other “health” message directed at either sex. 290,984 women died of cancer in 2018 with a little over 42,400 attributed to breast cancer. The rate of death from breast cancer is 25.5 per 100,000 women or 0.0255%.
On the other hand, circulatory disease, including heart disease and strokes, killed over 420,000 women in 2018. Myocardial infarction and atherosclerotic heart disease killed over 136,000 women in 2018 alone at a rate of 100.3 per 100,000 women (0.1%) or 4 times the number of deaths from breast cancer.
According to a systematic review of mammogram screening trials in the Cochrane Database, mammogram screening had an absolute risk reduction of 0.05% for breast cancer mortality. At the same time, absolute risk of overdiagnosis & overtreatment was 0.5%. In effect, for every 2,000 women screened throughout 10 years one will avoid dying from breast cancer while 10 healthy women will be treated unnecessarily.
Another study funded by the National Institute for Health Research (NIHR) Health Technology Assessment programme in the UK found a 25% risk reduction during the intervention phase at 10 year’s follow up. Sounds impressive.
Yet the absolute benefit was only 1 death from breast cancer was prevented for every 1,000 women screened. There was no effect on other-cause mortality.
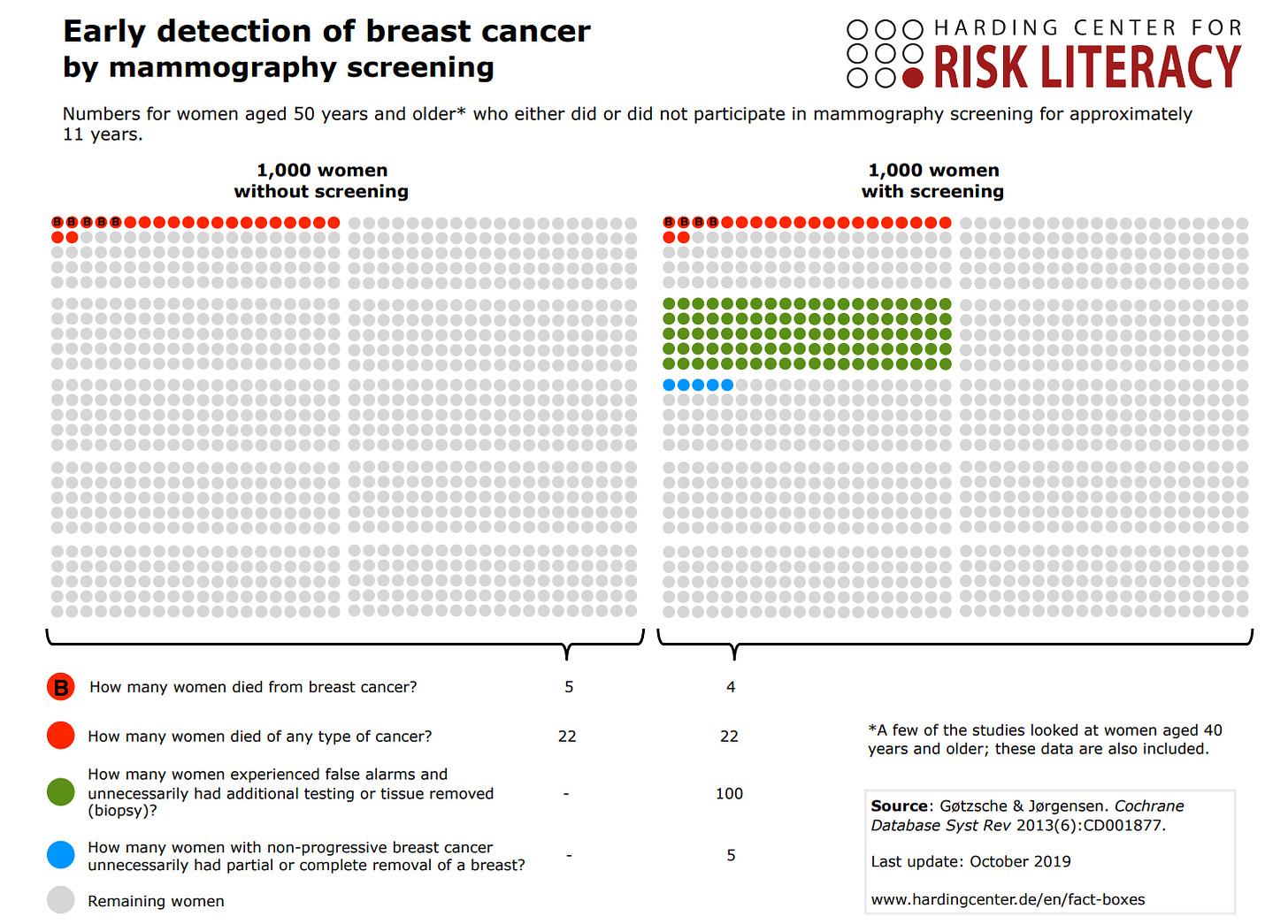
Here is another visual representation of the risks and benefits of breast cancer screening:
In addition to overdiagnosis and false-positives from mammograms, consider that mammography itself could cause breast cancer. Traditional mammograms emit about 7 weeks worth of radiation that a person typically receives on a daily basis directly into the breast in one sitting. 3D mammograms emit even higher doses.
Radiation is a known cause of cancer, and the radiation emitted during mammograms is being directed on an annual basis into the very tissue that the sick care community claims to want to protect. While there is no reliable evidence one way or the other, there is risk.
The drugs used to treat cancer also have very questionable efficacy due to issues surrounding the basic research upon which these drugs are developed. A former researcher from Amgen tried to reproduce the results of 53 landmark publications on cancer drug research, and found that they could not replicate the results of 47 out of the 53.
There are some interesting tidbits from this Reuters article.
Scientists at Bayer did not have much more success. In a 2011 paper titled, “Believe it or not,” they analyzed in-house projects that built on “exciting published data” from basic science studies. “Often, key data could not be reproduced,” wrote Khusru Asadullah, vice president and head of target discovery at Bayer HealthCare in Berlin, and colleagues.
Of 47 cancer projects at Bayer during 2011, less than one-quarter could reproduce previously reported findings, despite the efforts of three or four scientists working full time for up to a year. Bayer dropped the projects.
Bayer and Amgen found that the prestige of a journal was no guarantee a paper would be solid. “The scientific community assumes that the claims in a preclinical study can be taken at face value,” Begley and Lee Ellis of MD Anderson Cancer Center wrote in Nature. It assumes, too, that “the main message of the paper can be relied on ... Unfortunately, this is not always the case.”
and,
Part way through his project to reproduce promising studies, Begley met for breakfast at a cancer conference with the lead scientist of one of the problematic studies.
“We went through the paper line by line, figure by figure,” said Begley. “I explained that we re-did their experiment 50 times and never got their result. He said they’d done it six times and got this result once, but put it in the paper because it made the best story. It’s very disillusioning.”
Such selective publication is just one reason the scientific literature is peppered with incorrect results.
Tamoxifen is a drug that is supposed to prevent breast cancer from occurring or re-occurring. In this study published in the Journal of the National Cancer Institute, invasive breast cancer was reduced from 42.5 per 1,000 women in the control group to 24.8 per 1,000 in the treatment group. That is an absolute risk reduction of 1.7%
At the same time, for every 1,000 women who take tamoxifen, there were 5 additional cases of blood clots in their legs and lungs, and six more women got invasive uterine cancer. There was also no significant reduction in mortality from breast cancer or other causes.
What about the doctors?
So where are doctors in all of this? Unfortunately, most health professionals are just as uneducated about relative vs absolute risks and benefits as the average person. In Gigerenzer’s book, he refers to this as Innumeracy.
On top of that, the US is a highly litigious society and medical malpractice is incredibly lucrative for lawyers and patients if they win a case. This causes doctors to practice defensive medicine in which they will over-screen and over-treat in order to cover their asses saying they did all they could for a patient even when there is no discernible benefit.
Another problem is that we are witnessing the rise of a centralized, totalitarian medical regime that is stripping doctors of their licenses and board certifications as reprisal against those who choose not to follow the state determined narratives and treatment protocols. Several doctors including Dr. Peter McCullough, one of the top cardiologists in the world, is battling this right now due to his vocal opposition to the experimental gene therapies and ineffective COVID treatments such as Remdesivir.
The last problem is conflict of interest. Medical screenings and unnecessary treatments are incredibly profitable, and at the end of the day, our current sick care system is designed to maximize profits not health. Healthy people who don’t need to go to the doctor are not profitable.
As the saying goes, “Show me the incentive, and I will show you the behavior.” These medical screening procedures that are sold as “preventative” medicine are nothing of the sort.
While I'm sure the original intent was pure, they do not prevent anything. These screening tools are now used to recruit people who are often times perfectly healthy into a system that transfers wealth from patients to the sick care industry by prescribing medications and procedures that almost never address the underlying cause of disease.
So what is a person to do when accessing this broken healthcare system? Check out my next post “Navigating the Sick Care System” for some ideas.